Dementia with Lewy bodies (DLB) is a type of progressive dementia that leads to a decline in thinking, reasoning and independent function. Its features may include spontaneous changes in attention and alertness, recurrent visual hallucinations, REM sleep behavior disorder, and slow movement, tremors or rigidity.
About dementia with Lewy bodies
 Dementia with Lewy bodies is one of the causes of dementia, alongside other types of dementia like Alzheimer's disease and vascular dementia. "Lewy body dementia" (LBD) is a broad term that includes both dementia with Lewy bodies and Parkinson’s disease dementia. Here, we focus on the specific brain disorder called "dementia with Lewy bodies" (DLB).
Dementia with Lewy bodies is one of the causes of dementia, alongside other types of dementia like Alzheimer's disease and vascular dementia. "Lewy body dementia" (LBD) is a broad term that includes both dementia with Lewy bodies and Parkinson’s disease dementia. Here, we focus on the specific brain disorder called "dementia with Lewy bodies" (DLB).
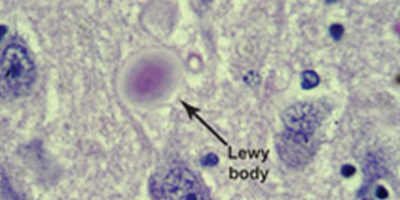
The hallmark brain abnormalities linked to DLB are named after Frederich H. Lewy, M.D., the neurologist who discovered them while working in Dr. Alois Alzheimer's laboratory during the early 1900s. Alpha-synuclein protein, the chief component of Lewy bodies, is found widely in the brain, but its normal function isn't yet known.
Lewy bodies may also be found in other types of dementia, including Alzheimer's disease dementia, and are a primary brain abnormality in Parkinson's disease dementia. Many people with Parkinson's eventually develop problems with thinking and reasoning, and many people with DLB experience movement symptoms like hunched posture, rigid muscles, a shuffling walk and trouble initiating movement.
This overlap in symptoms and other evidence suggest that dementia with Lewy bodies, Parkinson's disease, and Parkinson's disease dementia may be linked to the same underlying abnormalities in how the brain processes the protein alpha-synuclein. Many people with both DLB and Parkinson's dementia also have plaques and tangles — hallmark brain changes linked to Alzheimer's disease. When people have brain changes of more than one type of dementia, they are said to have mixed dementia.
Learn more: Mixed Dementia.
Symptoms of dementia with Lewy bodies
Core symptoms of dementia with Lewy bodies include:
- Changes in thinking and reasoning.
- Fluctuating cognition that is delirium-like.
- Recurrent well-formed visual hallucinations.
- REM sleep behavior disorder that involves acting out dreams.
- Spontaneous parkinsonism with slowness of movement, rest tremor, or rigidity.
Other symptoms may include:
- Trouble interpreting visual information.
- Malfunctions of the "automatic" (autonomic) nervous system, which controls automatic functions of the body, such as sweating, blood pressure, heart rate, digestion and sexual response.
- Memory loss that may be significant, but less prominent than in Alzheimer's.
Learn more about these and other possible symptoms from the
Lewy Body Dementia Association.
Diagnosis of dementia with Lewy bodies
Families facing dementia need you
Donate today so we can continue advancing critical research and providing free 24/7 support to those who depend on it.
Donate Now
As with other
types of dementia, there is no single test that can conclusively diagnose dementia with Lewy bodies. Today, DLB is a "clinical" diagnosis, which means it represents a doctor's best professional judgment about the reason for a person's symptoms. The only way to conclusively diagnose DLB is through a postmortem autopsy.
Most experts believe that dementia with Lewy bodies and Parkinson's disease dementia are two different expressions of the same underlying problems with brain processing of the protein alpha-synuclein. They recommend continuing to diagnose DLB and Parkinson's disease dementia as separate disorders.
- The diagnosis is DLB when a person experiences dementia either before, at the same time as, or within one year of the onset of symptoms of Parkinson’s disease. In some cases of DLB, symptoms of Parkinson’s disease, like changes in movement, may never occur.
- The diagnosis is Parkinson's disease dementia when a person experiences dementia at least one year (and usually several years) after the onset of symptoms of Parkinson’s disease. Parkinson's disease symptoms may include changes in movement like a tremor.
Since Lewy bodies usually coexist with Alzheimer's brain changes, it may sometimes be hard to distinguish DLB from Alzheimer's disease, especially in the early stages.
Key differences between Alzheimer's and dementia with Lewy bodies
- Memory loss tends to be a more prominent symptom in early Alzheimer's than in early DLB. However, advanced DLB may cause memory problems in addition to its more typical effects on judgment, planning and visual perception.
- Movement symptoms are more likely to be an important cause of disability early in DLB than in Alzheimer's. However, Alzheimer's can cause problems with walking, balance and getting around as it progresses to moderate and severe stages.
- Hallucinations and misidentification of familiar people are significantly more frequent in early-stage DLB than in Alzheimer's.
- REM sleep disorder is more common in early DLB than in Alzheimer's.
- Disruption of the autonomic nervous system — such as causing a blood pressure drop on standing, dizziness, falls and urinary incontinence — is much more common in early DLB than in Alzheimer's.
Causes and risks
Researchers have not yet identified any specific causes of dementia with Lewy bodies. Most people diagnosed with DLB have no family history of the disorder, and no genes linked to DLB have been conclusively identified.
Treatment and outcomes
There are no treatments that can slow or stop the brain cell damage caused by dementia with Lewy bodies. Current strategies focus on helping symptoms.
If your treatment plan includes medications, it's important to work closely with your physician to identify the drugs that work best for you and the most effective doses. Treatment considerations involving medications include the following issues:
- Cholinesterase inhibitor drugs are a common approach for addressing thinking changes in Alzheimer's. They also may help certain DLB symptoms.
- Antipsychotic drugs should be used with extreme caution in Lewy body dementia, including both dementia with Lewy bodies and Parkinson's disease dementia. Although physicians sometimes prescribe these drugs for behavioral symptoms that can occur in Alzheimer's, they may cause serious side effects in as many as 50% of those with Lewy body dementia. Side effects may include sudden changes in consciousness, impaired swallowing, acute confusion, episodes of delusions or hallucinations, or appearance or worsening of Parkinson's symptoms.
- Antidepressants may be used to treat depression, which is common with DLB, Parkinson's disease dementia and Alzheimer's. The most commonly used antidepressants are selective serotonin reuptake inhibitors (SSRIs).
Like other types of dementia that destroy brain cells, dementia with Lewy bodies gets worse over time and shortens lifespan.