
Triple Your Impact for Alzheimer's & Brain Awareness Month
Triple Your Impact for Alzheimer's & Brain Awareness Month
This is your moment to do more. Give by midnight on June 11 and your gift can be matched three times — up to $50,000 — to fund research, protect brain health and help provide care and support to those facing Alzheimer's disease.
Donate NowYou may remember, in a groundbreaking reveal last July at the Alzheimer’s Association International Conference (AAIC), it was announced that, for the first time, a large, randomized clinical trial – the SPRINT MIND study – showed that intensive treatment of high blood pressure (targeting a systolic blood pressure goal of less than 120 mm Hg) resulted in significantly fewer new cases of mild cognitive impairment (MCI).
MCI, which causes noticeable and measurable decline in cognitive abilities including memory and thinking skills, is a known risk factor for dementia. Everyone who experiences dementia passes through MCI. Therefore, when we prevent new cases of MCI, we are preventing new cases of dementia.
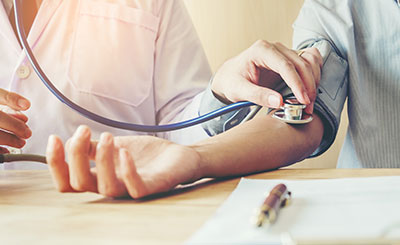 The findings from the SPRINT MIND study, published today in the Journal of the American Medical Association, are a clear indicator of a promising path to MCI prevention. However, the researchers were unable to follow the study participants for a long enough period of time to draw a decisive conclusion specifically about dementia. That's where the Alzheimer's Association comes in, to impact and drive critical research.
The findings from the SPRINT MIND study, published today in the Journal of the American Medical Association, are a clear indicator of a promising path to MCI prevention. However, the researchers were unable to follow the study participants for a long enough period of time to draw a decisive conclusion specifically about dementia. That's where the Alzheimer's Association comes in, to impact and drive critical research.With a financial commitment of more than $800,000, our investment will enable SPRINT MIND 2.0 to begin in early 2019. It will extend the follow up of a majority of the original SPRINT MIND trial participants and add an assessment to provide more definitive answers on how aggressively treating blood pressure may be key to preventing dementia.
Original Study Results
The SPRINT MIND study, which included 9,361 cognitively healthy older adults, compared two strategies for lowering blood pressure and measured the impact on MCI and dementia. One strategy was intensive blood pressure lowering (to 120mm Hg systolic) and the other was standard care at the time (lowering to 140mm Hg systolic).
In the group that received intensive blood pressure treatment, 19 percent less people developed mild cognitive impairment. That’s nearly one in five fewer people.
These findings are exciting because they show — more conclusively than ever before — that there are things we can do today, especially regarding cardiovascular disease risk factors, to reduce our risk of mild cognitive impairment. Talk to your doctor about controlling blood pressure, especially if you are age 50 or older. The conversation about healthy blood pressure management — and other heart and brain health issues — is one everyone should be having.
New Research = Hope
SPRINT MIND 2.0 provides genuine, concrete hope that we will have answers for future generations on how to prevent dementia.
The future of dementia prevention could very likely be in treating the whole person with a combination of drugs and modifiable lifestyle changes. We have seen these strategies help drive down death rates from cancer and heart disease. This is why the Alzheimer’s Association is leading the U.S. POINTER study to determine if a structured, coordinated, evidence-based recipe of lifestyle changes can protect cognitive function, including medical management of cardiovascular risk factors. These studies are critical pieces in this larger puzzle — and the results will deepen our understanding of brain health and move us closer to a world without Alzheimer’s disease.
About the author: As chief science officer, Maria C. Carrillo, Ph.D., sets the strategic vision for the Alzheimer’s Association global research program. Under her leadership, the Association is the world’s largest nonprofit funder of Alzheimer’s research.
Related articles:
Brain Health
Mild Cognitive Impairment (MCI)
