Be a Part of the Fight to End Alzheimer's
Be a Part of the Fight to End Alzheimer's
The millions of people impacted by this disease need your help. Your generosity can help us provide care and support to those facing the challenges of Alzheimer's and advance global research. Please make a gift today.
Donate NowDown Syndrome and Alzheimer's Disease
As they age, those affected by Down syndrome have a greatly increased risk of developing a type of dementia that's either the same as or very similar to Alzheimer's disease.
About Down syndrome and Alzheimer's
Down syndrome — also known as trisomy 21 — is a condition in which a person is born with extra genetic material from chromosome 21, one of the 23 human chromosomes. All human chromosomes usually occur in pairs, with one copy inherited from a person’s mother and one from the father. Most people with Down syndrome have a full extra copy of chromosome 21, and so they have three copies instead of the usual two. Scientists think the extra copy results from a random error in the specialized cell division that produces eggs and sperm.
Human chromosomes carry about 30,000 genes coding a person’s entire biological blueprint. Genes tell the body how to build proteins — the key molecules underlying all the body’s structures and functions. Researchers have so far identified more than 400 genes on chromosome 21, and they expect to find more.
In ways that scientists don't yet understand, the extra copies of genes present in Down syndrome cause developmental problems and health issues even though all three copies of the genes usually carry “normal” protein codes. Down syndrome nearly always affects learning, language and memory, but its impact varies from person to person. Other common health issues include heart defects present at birth, conditions affecting bones and muscles, and problems with vision and hearing. A core goal of Down syndrome research is to understand how the extra copy of chromosome 21 and its genes cause problems just by existing.
Advances in function, well-being and life span for people with Down syndrome have revealed an additional health risk: As they age, individuals affected by Down syndrome have a greatly increased risk of developing a type of dementia that’s either the same as or very similar to Alzheimer’s disease.
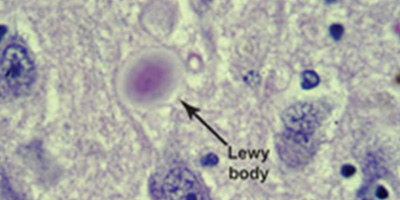
Autopsy studies show that by age 40, the brains of almost all individuals with Down syndrome have significant levels of beta-amyloid plaques and tau tangles, abnormal protein deposits considered Alzheimer's hallmarks. Despite the presence of these brain changes, not everyone with Down syndrome develops Alzheimer's symptoms.
One of the many questions researchers hope to answer about Down syndrome is why some people develop dementia symptoms and others don't. Researchers are working to answer a similar key question about those who don't have Down syndrome: Why do some people with brain changes characteristic of Alzheimer's never show symptoms of the disease?
Prevalence
As with all adults, advancing age also increases the chances a person with Down syndrome will develop Alzheimer's disease. According to the National Down Syndrome Society, about 30% of people with Down syndrome who are in their 50s have Alzheimer’s dementia. About 50% of people with Down syndrome in their 60s have Alzheimer’s dementia.
Causes and risk factors
Scientists don't yet know APP's function, but they've learned that day-to-day brain activity involves continuous "processing" of APP into shorter pieces. One of the brain's APP processing pathways produces beta-amyloid, a fragment that's the chief component of plaques and a prime suspect in Alzheimer's-related brain changes. Having an extra copy of the APP gene may increase production of beta-amyloid, triggering the chain of biological events leading to Alzheimer's.
The APP gene is also linked to Alzheimer's through its connection to rare inherited forms of Alzheimer’s disease. Certain small variations in the APP chemical code were the first genetic changes scientists identified that guarantee people will develop Alzheimer’s if they inherit such a change from either parent. Like other genetic variations that ensure a person will develop Alzheimer’s, these APP variations are extremely rare. Few, if any, people with Down syndrome have them.
The fact that APP is strongly implicated in Alzheimer's through two different mechanisms — one involving a whole extra copy of the normal gene and the other involving specific minor changes in the gene’s chemical code — makes the intersection of Down syndrome and Alzheimer's a strong focus of research.
Symptoms
In people with Down syndrome, changes in overall function, personality and behavior may be more common early signs of Alzheimer's than memory loss and forgetfulness.
Early symptoms may include:
- Reduced interest in being sociable, conversing or expressing thoughts.
- Decreased enthusiasm for usual activities.
- Decline in ability to pay attention.
- Sadness, fearfulness or anxiety.
- Irritability, uncooperativeness or aggression.
- Restlessness or sleep disturbances.
- Seizures that begin in adulthood.
- Changes in coordination and walking.
- Increased noisiness or excitability.
Diagnosis
Most adults with Down syndrome will not self-report concerns about memory. Diagnosing dementia in a person with Down syndrome can be difficult because of the challenges involved in assessing thinking-skill changes in those with intellectual disabilities.
Yet, recognition of adult cognitive change is important for providing appropriate services and support for individuals with Down syndrome and their caregivers. Experts recommend the following principles as key to person-centered diagnosis in those with Down syndrome:
- Document baseline adult function by age 35. Ongoing evaluation of intellectual, behavioral and social function is important for everyone with Down syndrome. By age 35, each individual's medical record should ideally include detailed information on his or her adult abilities. The person with Down syndrome, family members, and other reliable individuals are helpful sources for this information.
- Watch for changes in day-to-day function. Reduced enthusiasm for daily activities, loss of interest in social interactions, and changes in personality and behavior are often early signs of an underlying decline in thinking skills.
- Consider professional assessment by a dementia expert. A variety of cognitive tests have been used to evaluate thinking changes in adults with Down syndrome. However, experts caution that cognitive tests should never be used as the only benchmark to diagnose dementia.
- Rule out other causes of symptoms. It’s important to rule out other medical conditions commonly associated with Down syndrome as the cause of changes in thinking and function, including thyroid problems, depression, chronic ear and sinus infections, vision loss, and sleep apnea.
Outcomes
Despite modern improvements in quality and length of life, Down syndrome remains a condition that shortens life span. People with Down syndrome experience earlier-than-usual onset of a variety of conditions linked to aging in addition to Alzheimer's disease. People with Down syndrome currently live an average of 60 years, although some live into their seventies and, rarely, into their eighties.Treatment
The U.S. Food and Drug Administration (FDA) has not approved any drugs specifically to treat dementia associated with Down syndrome. In the United Kingdom, cholinesterase inhibitors, a class of drugs approved in the United States and many other countries to treat Alzheimer's, are approved to treat dementia in people with Down syndrome. An analysis by the Cochrane Reviews, an extensive series of reports by international experts evaluating treatment effectiveness, found that there isn’t enough evidence to reach a conclusive judgment about the benefit of cholinesterase inhibitors for people with Down syndrome.
An international randomized trial has shown no benefit for the Alzheimer's drug memantine in adults with Down syndrome. Experts urge more research and clinical studies to identify effective treatments for dementia in those with Down syndrome. Because there may be differences in the way people with Down syndrome process medications, experts advise caution about using any drug that has not specifically been shown to be safe and effective in this group.
Research
In November 2015, the National Institutes of Health launched a $37 million initiative to identify biomarkers in the blood and brain that can help identify and track Alzheimer’s in people with Down syndrome. The Alzheimer’s Association, the Linda Crnic Institute for Down Syndrome and the Global Down Syndrome Foundation convened scientific workshops addressing Alzheimer’s and Down syndrome, and are funding efforts to develop a blood test to identify individuals at high risk for developing Alzheimer’s.
In October 2017, Biogen committed more than $500,000 and additional in-kind resources to the Crnic Institute to investigate the genome and epigenome of specific cell types in the blood that could inform the development of Alzheimer’s disease.
Find a complete list of Alzheimer’s trials involving people with Down syndrome.
Help is available
National Down Syndrome Society (NDSS) is a nonprofit organization that offers information and support to individuals with Down syndrome and their families. Call NDSS at 800.221.4602 or view their Aging and Down Syndrome: A Health & Well-Being Guidebook online.
The National Association for Down Syndrome (NADS) educates the public and offers information and support to people living with Down syndrome and their families.
A nonprofit dedicated to improving the lives of people with Down syndrome, the Global Down Syndrome Foundation supports the Linda Crnic Institute for Down Syndrome, which focuses on research and medical care for those with Down syndrome.
The National Down Syndrome Congress (NDSC) raises awareness and advocates for those impacted by Down syndrome.
The Alzheimer's Association can help you learn more about Alzheimer's disease and other dementias, and help you find local support services. Call our 24/7 Helpline at 800.272.3900.
Related Pages
The Alzheimer’s Association is in your community.
Find Your Local Chapter
Learn how Alzheimer’s disease affects the brain.
Take the Brain Tour