This Month, You Can Double Your Impact
This Month, You Can Double Your Impact
You can make twice the difference during Alzheimer’s & Brain Awareness Month with our Double Your Impact Match Challenge — but only until June 8. Your gift can go twice as far to help provide care and support and advance research.
Donate NowPosterior Cortical Atrophy
Posterior cortical atrophy (PCA) refers to gradual and progressive degeneration of the outer layer of the brain (the cortex) in the part of the brain located in the back of the head (posterior).
About posterior cortical atrophy
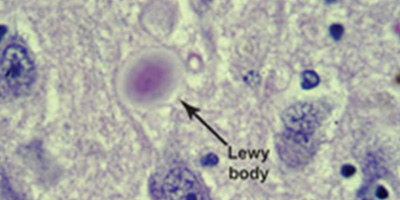
 It is not known whether posterior cortical atrophy is a unique disease or a possible variant form of Alzheimer’s disease. In many people with posterior cortical atrophy, the affected part of the brain shows amyloid plaques and neurofibrillary tangles, similar to the changes that occur in Alzheimer’s disease but in a different part of the brain. In other people with posterior cortical atrophy, however, the brain changes resemble other diseases such as dementia with Lewy bodies or a form of Creutzfeldt-Jakob disease. Most cases of Alzheimer’s disease occur in people age 65 or older, whereas the onset of posterior cortical atrophy commonly occurs between ages 50 and 65.
It is not known whether posterior cortical atrophy is a unique disease or a possible variant form of Alzheimer’s disease. In many people with posterior cortical atrophy, the affected part of the brain shows amyloid plaques and neurofibrillary tangles, similar to the changes that occur in Alzheimer’s disease but in a different part of the brain. In other people with posterior cortical atrophy, however, the brain changes resemble other diseases such as dementia with Lewy bodies or a form of Creutzfeldt-Jakob disease. Most cases of Alzheimer’s disease occur in people age 65 or older, whereas the onset of posterior cortical atrophy commonly occurs between ages 50 and 65.
Prevalence
There is no standard definition of posterior cortical atrophy and no established diagnostic criteria, and so it is not possible to know how many people have the condition. Some studies have found that about 5 percent of people diagnosed with Alzheimer’s disease have posterior cortical atrophy. However, because posterior cortical atrophy often goes unrecognized, the true percentage may be as high as 15 percent.
Symptoms
The symptoms of posterior cortical atrophy can vary from one person to the next and can change as the condition progresses. The most common symptoms are consistent with damage to the posterior cortex of the brain, an area responsible for processing visual information. Consistent with this neurological damage are slowly developing difficulties with visual tasks such as reading a line of text, judging distances, distinguishing between moving objects and stationary objects, inability to perceive more than one object at a time, disorientation, and difficulty maneuvering, identifying, and using tools or common objects. Some patients experience hallucinations. Other symptoms can include difficulty performing mathematical calculations or spelling, and many people with posterior cortical atrophy experience anxiety, possibly because they know something is wrong. In the early stages of posterior cortical atrophy, most people do not have markedly reduced memory, but memory can be affected in later stages.
Diagnosis
Misdiagnosis of posterior cortical atrophy is common, owing to its relative rarity and unusual and variable presentation. Additionally, people with posterior cortical atrophy frequently first seek the opinion of an ophthalmologist who may indicate a normal eye examination by their usual tests. Because the first problems are perceived as eye problems, cortical brain dysfunction initially may not be considered as a cause.
Physicians rely on a combination of neuropsychological tests, blood tests, brain scans and a neurological examination to diagnose the condition and rule out other potential explanations for symptoms. Characteristic features that are sometimes used for diagnosis include gradual onset of visual symptoms (described above) with preservation of normal eye function and preservation of memory. Age of onset between 50 and 65 years is another clue suggesting PCA. The diagnosis should rule out the possibility that the symptoms were caused by a stroke, tumor or other identifiable condition.
There is an ongoing discussion in the field whether posterior cortical atrophy should be considered a form of Alzheimer’s disease or a distinct disease entity. Brain imaging has shown that the posterior cortex is thinner in people with posterior cortical atrophy than healthy people of the same age. This indicates that the individual has experienced a decrease in brain volume. Furthermore, people with posterior cortical atrophy have degeneration in different parts of the brain than people with typical forms of Alzheimer’s disease, although there is often overlap between the two conditions.
Causes and risks
Similar to Alzheimer’s disease, the causes of posterior cortical atrophy are unknown, and no obvious genetic mutations have been shown to be linked to the condition. It is also not known if the risk factors for Alzheimer’s disease are also risk factors for posterior cortical atrophy.
Treatment and outcomes
There are no treatments for posterior cortical atrophy known to slow or halt its progression. Because posterior cortical atrophy resembles Alzheimer’s disease in some patients, it has been suggested that drugs used to temporarily alleviate brain dysfunction in Alzheimer’s disease may be helpful in posterior cortical atrophy, but this is not proven. Some people with posterior cortical atrophy may benefit from treatment to alleviate symptoms such as depression or anxiety, but the overall benefits and risks of such treatments are not established.
Related Pages
The Alzheimer’s Association is in your community.
Find Your Local Chapter
Learn how Alzheimer’s disease affects the brain.
Take the Brain Tour