Be a Part of the Fight to End Alzheimer's
Be a Part of the Fight to End Alzheimer's
The millions of people impacted by Alzheimer's disease need your help. Your generosity can help us provide care and support to these facing the challenges of Alzheimer's, protect brain health and advance global research. Please make a gift today.
Donate NowKorsakoff Syndrome
Korsakoff syndrome is a chronic memory disorder caused by severe deficiency of thiamine (vitamin B-1). Korsakoff syndrome is most commonly caused by alcohol misuse, but certain other conditions also can cause the syndrome.
About Korsakoff syndrome
Thiamine helps brain cells produce energy from sugar. When levels fall too low, brain cells cannot generate enough energy to function properly. Korsakoff syndrome is most commonly caused by alcohol misuse, but can also be associated with AIDS, cancers that have spread throughout the body, chronic infections, poor nutrition and certain other conditions. It is also common in people whose bodies do not absorb food properly (malabsorption). This can sometimes occur with a chronic illness or after weight-loss (bariatric) surgery. See causes and risk factors below.
Alcohol misuse and cognitive decline
Korsakoff syndrome and its associated thiamine deficiency is not the only mechanism through which heavy drinking may contribute to chronic thinking changes and cognitive decline. Alcohol misuse also may lead to brain damage through:
- The direct toxic effects of alcohol on brain cells.
- The biological stress of repeated intoxication and withdrawal.
- Alcohol-related cerebrovascular disease.
- Head injuries sustained when inebriated.
Korsakoff syndrome is often — but not always — preceded by an episode of Wernicke encephalopathy, which is an acute brain reaction to severe lack of thiamine. Wernicke encephalopathy is a medical emergency that causes life-threatening brain disruption, confusion, staggering and stumbling, lack of coordination, and abnormal involuntary eye movements.
Because the chronic memory loss of Korsakoff syndrome often follows an episode of Wernicke encephalopathy, the chronic disorder is sometimes known as Wernicke-Korsakoff syndrome. But Korsakoff syndrome can also develop in individuals who have not had a prior episode of Wernicke encephalopathy.
Prevalence
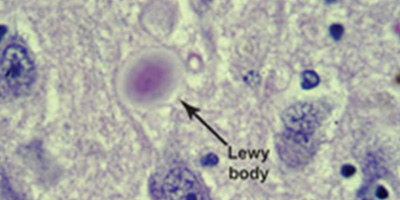
Scientists don’t know exactly how many people have Korsakoff syndrome. It’s widely considered less common than Alzheimer’s disease, vascular dementia, frontotemporal dementia or dementia with Lewy bodies. Like more common types of dementia, it may be underdiagnosed.
Causes and risk factors
Scientists don't yet know exactly how Korsakoff syndrome damages the brain. Research has shown that severe thiamine deficiency disrupts several biochemicals that play key roles in carrying signals among brain cells and in storing and retrieving memories. These disruptions destroy brain cells and cause widespread microscopic bleeding and scar tissue. Researchers have identified several genetic variations that may increase susceptibility to Korsakoff syndrome. Poor nutrition also may raise risk.
Most cases of Korsakoff syndrome result from alcohol misuse. Scientists don't yet know why heavy drinking causes severe thiamine deficiency in some alcoholics, while others may be affected primarily by alcohol's effects on the liver, stomach, heart, intestines or other body systems. Sign up for our e-news to receive updates about Alzheimer’s and dementia care and research.
Korsakoff syndrome may sometimes be associated with disorders other than alcohol misuse, including anorexia, overly stringent dieting, fasting, starvation or weight-loss surgery; uncontrolled vomiting; AIDS; kidney dialysis; chronic infection; or cancer that has spread throughout the body.
Symptoms
Korsakoff syndrome causes problems learning new information, inability to remember recent events and long-term memory gaps. Memory difficulties may be strikingly severe while other thinking and social skills are relatively unaffected. For example, individuals may seem able to carry on a coherent conversation but moments later are unable to recall that the conversation took place or with whom they spoke.
Those with Korsakoff syndrome may "confabulate," or make up, information they can't remember. They are not "lying" but may actually believe their invented explanations. Scientists don’t yet understand the mechanism by which Korsakoff syndrome may cause confabulation. The person may also see or hear things that are not there (hallucinations).
Diagnosis
Experts recommend that a medical workup for memory loss or other cognitive changes always include questions about an individual's alcohol use. Anyone admitted to the hospital for an alcohol-related condition should be professionally screened for memory loss and cognitive change. The screening should include supplementary questions to assess recent memory. If screening suggests impairment, the person should receive a more detailed cognitive workup.
Outcomes
Wernicke encephalopathy, a related disorder that sometimes precedes Korsakoff syndrome, is a medical emergency. Untreated, it causes death in up to 20 percent of cases and progresses to Korsakoff syndrome in 85 percent of survivors. Abnormal eye movements that occur in Wernicke encephalopathy may respond to injectable thiamine within a few days. Lack of coordination and clumsiness may begin to improve after about a week but may take several months to clear up completely. Confusion also takes several months to clear up. As confusion clears, the severe memory problems associated with Korsakoff syndrome may become more noticeable.
In those who develop Korsakoff syndrome with or without a preceding episode of Wernicke encephalopathy, there are few studies on long-term outcomes. Available data suggest that about 25 percent of those who develop Korsakoff syndrome eventually recover, about half improve but don’t recover completely, and about 25 percent remain unchanged. Some research suggests that those who recover from an episode may have a normal life expectancy if they abstain from alcohol.
Treatment
Some experts recommend that heavy drinkers and others at risk of thiamine deficiency take oral supplements of thiamine and other vitamins under their doctor’s supervision.
Many experts also recommend that anyone with a history of heavy alcohol use who experiences symptoms associated with Wernicke encephalopathy, including acute confusion, prolonged nausea and vomiting, unusual fatigue or weakness, or low body temperature or blood pressure, be given injectable thiamine until the clinical picture grows clearer.
Once acute symptoms improve, individuals should be carefully evaluated to determine if their medical history, alcohol use and pattern of memory problems may be consistent with Korsakoff syndrome. For those who develop Korsakoff syndrome, extended treatment with oral thiamine, other vitamins and magnesium may increase chances of symptom improvement. If there is no improvement, consideration should be given to treatment of comorbid deficiencies and medical conditions, and the need for long-term residential care or supportive accommodation.
Abstaining from alcohol and maintaining a healthy diet is a cornerstone of effective long-term treatment. Those with Korsakoff syndrome have a reduced tolerance for alcohol and may be at high risk for further alcohol-related health problems.
Help is available
The Alzheimer's Association can help you learn more about Alzheimer's disease and other dementias, and help you find local support services. Call our 24/7 Helpline at 800.272.3900.
National Institute on Alcohol Abuse and Alcoholism (NIAAA) supports and conducts research on the impact of alcohol use on human health and well-being.
Family Caregiver Alliance (FCA) has information about Wernicke-Korsakoff syndrome on their website. FCA provides caregivers programs to support families and friends caring for loved ones with chronic, disabling health conditions. Call FCA at 800.445.8106.
Related Pages
The Alzheimer’s Association is in your community.
Find Your Local Chapter
Learn how Alzheimer’s disease affects the brain.
Take the Brain Tour