Make Twice the Impact with Our Spring Match Challenge
Make Twice the Impact with Our Spring Match Challenge
Help us fight Alzheimer’s and deliver twice the help and hope during our Spring 2x Match Challenge. Your gift will advance research and help provide care and support for the millions affected by Alzheimer’s.
Donate NowMedical Tests for Diagnosing Alzheimer's
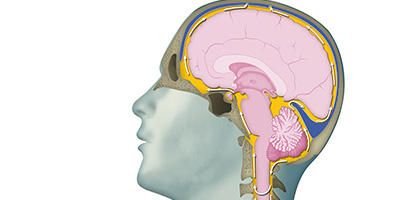
There is no single test that can determine if a person is living with Alzheimer’s or another dementia. Physicians use diagnostic tools combined with medical history and other information, including neurological exams, cognitive and functional assessments, brain imaging (MRI, CT, PET) and cerebrospinal fluid or blood tests to make an accurate diagnosis.
Medical history
During the medical workup, the health care provider will review the person's medical history, including psychiatric history and history of cognitive and behavioral changes. He or she will want to know about any current and past medical problems and concerns, as well as any medications the person is taking. The doctor will also ask about key medical conditions affecting other family members, including whether they may have had Alzheimer's disease or other dementias.
Physical exam and diagnostic tests
During a medical workup, the physician will likely:
What to expect
Take our interactive tour to learn what to expect when being evaluated for memory and thinking problems.
- Ask about diet, nutrition and use of alcohol.
- Review all medications. (Bring a list or the containers of all medicines currently being taken, including over-the-counter drugs and supplements.)
- Check blood pressure, temperature and pulse.
- Listen to the heart and lungs.
- Perform other procedures to assess overall health.
- Collect blood or urine samples for laboratory testing.
Information from a physical exam and laboratory tests can help identify health issues that can cause symptoms of dementia. Common causes of dementia-like symptoms are depression, untreated sleep apnea, delirium, side effects of medications, thyroid problems, certain vitamin deficiencies and excessive alcohol consumption. Unlike Alzheimer’s and other dementias, these conditions often may be reversed with treatment.
If the diagnosis is Alzheimer’s or another dementia, you or your loved one are not alone. Join our free online community ALZConnected to share questions, experiences and practical tips on message boards and in live chat rooms.
Be prepared for the doctor to ask:
- What kind of symptoms have you noticed?
- When did they begin?
- How often do they happen?
- Have they gotten worse?
The doctor may also ask a family member to provide input about changes in your thinking skills and behavior. See our Communicating with Doctors or Health Care Professionals (PDF) to get ready for your appointment.
Neurological exam
During a neurological exam, the physician will closely evaluate the person for problems that may signal brain disorders other than Alzheimer's. The doctor will look for signs of stroke, Parkinson's disease, brain tumors, buildup of fluid in the brain, and other conditions that may impair memory or thinking.
The physician will test:
- Reflexes
- Coordination, muscle tone and strength
- Eye movement
- Speech
- Sensation
The neurological exam may also include a brain imaging study.
If the evaluation does not indicate Alzheimer's disease or another dementia, but the symptoms continue to get worse over time, your doctor may need to order more tests, or you may wish to get a second opinion.
Learn more: What Is Alzheimer's?, What Is Dementia? and Types of Dementia.
Home screening tests for dementia
A number of dementia screening tests have been marketed directly to consumers. None of these tests have been scientifically proven to be accurate. Furthermore, the tests can have false-positive results, meaning that individuals can have results saying they have dementia when in fact they do not. This is extremely unlikely to happen if the individual visits a physician to seek care and potential diagnosis. For these and other reasons, the Alzheimer's Association believes that home screening tests cannot and should not be used as a substitute for a thorough examination by a skilled doctor. The whole process of assessment and diagnosis should be carried out within the context of an ongoing relationship with a responsible and qualified health care professional.
Cognitive, functional and behavioral tests
Cognitive, functional and behavioral tests evaluate memory, thinking and simple problem-solving abilities, and may quickly assess changes in behaviors and symptoms. Some tests are brief, while others can be more time intensive and complex. More comprehensive cognitive, functional and behavioral tests are often given by a neuropsychologist to evaluate executive function, judgment, attention and language.
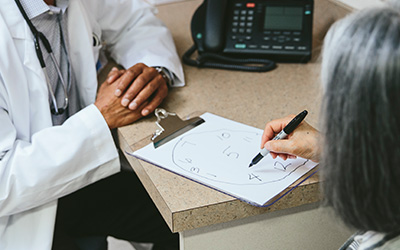
Such tests may give an overall sense of whether a person is experiencing cognitive symptoms that affect activities of daily living and function and is aware of these symptoms; knows the date, time and where he or she is; and can remember a short list of words, follow instructions and perform simple calculations.
Examples of cognitive, functional and behavioral tests include:
- Ascertain Dementia 8 (AD8)
- Saint Louis University Mental Status (SLUMS)
- The Informant Questionnaire on Cognitive Decline in the Elderly (IQCODE or s-IQCODE)
- Functional Activities Questionnaire (FAQ)
- Mini-Mental State Exam (MMSE)
Computerized cognitive tests and devices
A growing area of research is the development of medical devices and technologies to help physicians evaluate cognition and function. Among these are medical devices or digital technologies including computerized testing software; these have several advantages, including giving tests exactly the same way each time.Digital computerized assessments are designed to measure an individual's performance on a variety of cognitive or functional tasks and may be appropriate for administration in randomized clinical trials or clinical settings, when lengthier standard assessments are not practical.
The U.S. Food and Drug Administration (FDA) has cleared several digital cognitive testing tools for marketing:
- Automated Neuropsychological Assessment Metrics (ANAM)
- Cambridge Neuropsychological Test Automated Battery (CANTAB Mobile®)
- CognICA
- Cognigram
- Cognivue
Depression screen and mood assessment
In addition to assessing mental status, the doctor will evaluate a person's sense of well-being to detect depression or other mood disorders that can cause memory problems, loss of interest in life, and other symptoms that can overlap with dementia.
Genetic testing
Researchers have identified certain genes that increase the risk of developing Alzheimer's and other rare "deterministic" genes that directly cause Alzheimer's. Although genetic tests are available for some of these genes, health professionals do not currently recommend routine genetic testing for Alzheimer's disease.
Risk genes: While there is a blood test for APOE-e4, the strongest risk gene for Alzheimer's, this test is mainly used in clinical trials to identify people at higher risk of developing Alzheimer's. Carrying this gene mutation only indicates a greater risk; it does not indicate whether a person will develop Alzheimer's or whether a person has Alzheimer's. Genetic testing for APOE-e4 is controversial and should only be undertaken after discussion with a physician or genetic counselor.
Deterministic genes: Testing also is available for genes that cause autosomal dominant Alzheimer's disease (ADAD) or "familial Alzheimer's," a rare form of Alzheimer's that accounts for 1 percent or less of all cases. ADAD runs strongly in families and tends to begin earlier in life, sometimes as early as one’s 30s. Many people in these families do not wish to know their genetic status, but some get tested to learn whether they will eventually develop the disease. Some ADAD families have joined clinical studies to help researchers better understand Alzheimer's.
Learn more: Genetic Testing Fact Sheet (PDF) and Genetics and Alzheimer's.
Brain imaging
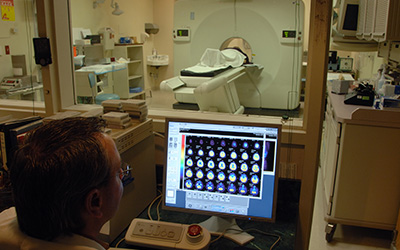 A standard medical workup for Alzheimer's disease often includes structural imaging with magnetic resonance imaging (MRI) or computed tomography (CT). These tests are primarily used to rule out other conditions that may cause symptoms similar to Alzheimer's but require different treatment. Structural imaging can reveal tumors, evidence of small or large strokes, damage from severe head trauma, or a buildup of fluid in the brain.
A standard medical workup for Alzheimer's disease often includes structural imaging with magnetic resonance imaging (MRI) or computed tomography (CT). These tests are primarily used to rule out other conditions that may cause symptoms similar to Alzheimer's but require different treatment. Structural imaging can reveal tumors, evidence of small or large strokes, damage from severe head trauma, or a buildup of fluid in the brain.
In some circumstances, a doctor may use brain imaging tools to find out if the individual has high levels of beta-amyloid, a hallmark of Alzheimer’s; normal levels would suggest Alzheimer’s is not the cause of dementia.
Imaging technologies have revolutionized our understanding of the structure and function of the living brain. Researchers are studying other brain imaging techniques so they can better diagnose and track the progress of Alzheimer’s.
Cerebrospinal fluid (CSF) tests
CSF is a clear fluid that bathes and cushions the brain and spinal cord. Adults have about 1 pint of CSF, which physicians can sample through a minimally invasive procedure called a lumbar puncture, or spinal tap. Research suggests that Alzheimer's disease in early stages may cause changes in CSF levels of multiple markers such as tau and beta-amyloid, two markers that form abnormal brain deposits strongly linked to Alzheimer's. Another potential marker is neurofilament light (NfL), an increased level of which has been found in neurodegenerative diseases such as Alzheimer’s.
One challenge researchers face is that analysis of biomarker levels in the same sample can often vary significantly from institution to institution and across different testing platforms. Great strides have been made in standardizing the measurement of these markers in research and clinical care. CSF tests are currently used by dementia specialists to aid in the diagnosis of Alzheimer's, and research continues to develop and standardize new markers that will aid in diagnosis and detection of other dementias.
There are a few new CSF tests — Lumipulse® and Elecsys® — that have received FDA approval. These diagnostic tools can be used by clinicians to detect beta-amyloid and tau markers in CSF, which can be predictive of amyloid changes in the brain.
The Alzheimer's Association convened a multidisciplinary workgroup and published appropriate use criteria to guide the safe and optimal use of the lumbar puncture procedure and CSF testing for Alzheimer's disease.
Blood tests
Researchers are investigating whether consistent and measurable changes in blood levels of specific markers may be reliably associated with Alzheimer's related changes. These markers may include tau, beta-amyloid or other biomarkers that could be measured before and after symptoms appear.
An urgent need exists for simple, inexpensive, non-invasive and easily available diagnostic tools such as blood tests to diagnose the disease. Some blood tests are already being used in many doctors' offices and clinics. It's important to discuss the pros and cons of blood testing with your doctor, who can take your specific situation into consideration.
The best blood tests are very accurate and can help find signs of Alzheimer's early, allowing for further testing to confirm diagnosis sooner. To support informed decisions, there should also be a clear plan for what happens next if the blood test shows signs of Alzheimer's.
To help strengthen how these tests are used in everyday care, the Alzheimer's Association and its partners are studying how blood tests work in many different types of clinics with different kinds of people. The Association is also putting more funding into research to make sure we get strong, reliable results about how these blood tests should be used.
In July 2025, the Association formally published an evidence-based clinical practice guideline on the use of blood-based biomarker testing to diagnose Alzheimer's disease in specialty care settings.