This blog is by Kristen Clifford, chief program officer, Alzheimer’s Association, and
Dennis J. Selkoe, M.D., Coates Professor of Neurologic Diseases, Harvard Medical School and Brigham and Women’s Hospital.
Early June headlines only hinted at the significance of the event: On June 7, the U.S. Food and Drug Administration (FDA) granted accelerated approval of a new drug, aducanumab (Aduhelm), to treat Alzheimer’s disease at the mild cognitive impairment or mild dementia stage. It was the first new FDA-approved treatment for Alzheimer’s in nearly 20 years.
The real story — the historic news that more than 6 million Americans living with the disease and their families had been waiting for — was largely missed: Aduhelm is the first approved treatment to attempt to change the underlying course of the disease, giving people with early Alzheimer’s and their families the possibility of more time to maintain their memories and thinking abilities.
Simply put: The availability of a new drug signals a new day in Alzheimer’s treatment.
Doctors’ phones are ringing, their in-boxes full of hopeful questions. This new treatment is spurring conversations between families, and between patients and doctors — all eager to learn about options that were never available before.
But hopeful families are encountering a major roadblock. While this new treatment is within reach, its availability and coverage remain elusive.
Alzheimer’s is a fatal disease. This new treatment option and related treatments on the horizon are a medical necessity. New treatments — and the steps that go along with administering them, according to their drug labels — should be covered by Medicare and other insurers.
The Alzheimer’s Association is working with experts in the field to develop guiding principles for people in all communities to access high quality care and treatment, in order to better manage and potentially slow the progression of the disease.
More treatments in this class of therapies are on the way.
Donanemab, one of the anti-amyloid treatments in the pipeline, received
Breakthrough Therapy designation from the FDA in June 2021. Eli Lilly stated “preliminary clinical evidence indicates that the drug may demonstrate substantial improvement on a clinically significant endpoint(s) over already available therapies that have received full FDA approval.” In a phase 2 clinical trial of people with early Alzheimer’s, donanemab cleared beta amyloid plaques from the brain and slowed the decline of memory, thinking and daily activities.
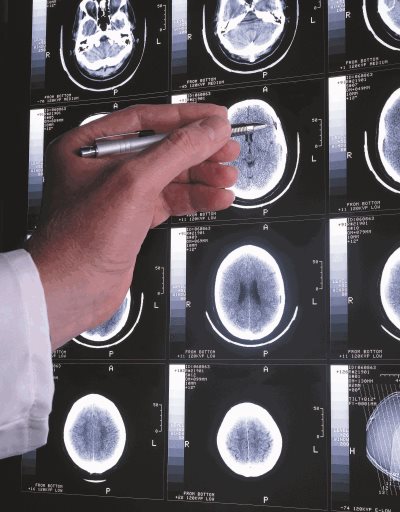
In addition to clearing beta amyloid, donanemab also showed less
tau progression in the brains of select patients, yet another important development following the FDA approval of Aduhelm.
Donamemab isn’t the only new potential treatment on the horizon. Another monoclonal antibody,
lecanemab, received Breakthrough Therapy designation from the FDA in June. Meanwhile, a fourth drug of this type,
gantenerumab, is also in advanced clinical trials.
With new and improved drugs under development every day, this is just the beginning.
These anti-amyloid drugs are not a cure; they are showing us how to slow, modify or change a disease that continues to devastate families and communities around the world.
Despite calls to action to ensure that health care is accessible and equal for all, that aim is still far from reality for many Americans, as the Alzheimer’s Association Race, Ethnicity and Alzheimer’s in America special report shows. We need to move toward combination therapies that work effectively across the entire course of the disease, and for all those living with Alzheimer’s. And this is already happening in research labs across the globe, funded by visionary organizations, governments and philanthropists.
Just two years ago, the outlook on Alzheimer’s drugs was grave. By the end of 2019, several companies slowed down their research into new drugs for Alzheimer’s. It looked like the pipeline might run dry. It didn’t, in part because nonprofits like the Alzheimer’s Association and government agencies kept the research dollars continuously flowing. Today, nearly half of Alzheimer’s treatment clinical trials in the U.S. are funded by nonprofits and the government, including important very early phase (presymptomatic) studies and investigations into drugs already approved for other diseases.
Still, let’s be clear about the stakes: Today, no one survives Alzheimer’s, and without medical breakthroughs, the number of Americans age 65 and older with Alzheimer’s dementia is forecast to double to more than 12 million by 2050. Aduhelm’s label indicates that it should only be prescribed for people with mild cognitive impairment and mild dementia due to Alzheimer’s disease, so it might seem like the drug’s FDA approval is only an incremental movement in the fight to end Alzheimer’s.
But it’s so much more than that. Much like the turn of the tide in cancer and HIV years ago, it means more and better treatments are on the way. And for the millions affected, there is hope.
About: Kristen Clifford is chief program officer at the Alzheimer’s Association. Dennis J. Selkoe, M.D., Harvard Medical School and Brigham and Women’s Hospital, is author of a recent Perspective published in Science, "Treatments for Alzheimer’s disease emerge," which evaluates aducanumab and several other innovative anti-amyloid treatment approaches that are now in the pipeline and advancing quickly.
DISCLOSURE
Dr. Selkoe a director of and consultant for Prothena Biosciences.
Related articles:
Research and Progress
Alzheimer's Association Funded Studies
Our Commitment to Global Research
Part the Cloud
Alzheimer’s Advocacy